What if the “minimally invasive” label you’ve heard for years was actually just the beginning of what’s possible for your back pain? You’ve likely exhausted conservative care and still face daily frustration, yet the fear of a long hospital stay or permanent muscle damage keeps you from seeking surgical help. It’s understandable to feel hesitant when traditional methods seem so aggressive. Discover how 2026 advancements in endoscopic spine surgery offer a sophisticated alternative that prioritizes your quality of life and reduces the risk of infection by nearly six times compared to open surgery. You’ll learn how modern outpatient protocols in Plano and Lewisville allow for smaller incisions, minimal scarring, and a return to normal activity within weeks. We’ll explore the shift toward ambulatory surgical centers and how these precise interventions provide the relief you’ve been searching for without the need for spinal fusion.
Key Takeaways
- Explore the technology behind HD camera-guided procedures that allow for targeted relief through a 1/4-inch incision.
- Compare the benefits of muscle-sparing approaches against traditional surgery to see how tissue preservation accelerates healing.
- Determine if you are a candidate for endoscopic spine surgery by identifying which spinal conditions respond best to this advanced intervention.
- Map out your recovery timeline and learn how our specialized protocols help you achieve a rapid return to normal activity.
- Understand the importance of surgeon specialization and the advantages of receiving care in a personalized, high-tech boutique environment.
What is Endoscopic Spine Surgery? The Ultra-Minimally Invasive Standard
Endoscopic spine surgery represents the absolute pinnacle of modern surgical innovation. It’s often referred to as “ultra-minimally invasive” because it goes several steps beyond traditional techniques to protect the patient’s anatomy. Dr. Scott Kutz has been a pioneer in bringing these advanced methods to the Plano and Lewisville communities, providing a high-tech alternative for those who want to avoid the trauma of open back surgery. The goal is simple yet profound: treat the underlying condition with surgical precision while leaving the surrounding healthy tissue untouched.
The primary difference lies in the access point. While traditional surgery may require large incisions that disrupt significant muscle groups, this approach uses an incision only 1/4 inch wide. This is roughly the size of a pencil eraser. Because the surgeon doesn’t need to cut or strip major back muscles to reach the spine, the physical impact on your body is drastically reduced. This philosophy is a key part of the broader field of Minimally Invasive Spine Surgery, which focuses on achieving the same therapeutic goals as open surgery with far less collateral damage. By avoiding muscle trauma, patients experience significantly less post-operative pain and a much faster healing process.
The Technology Behind the Tiny Incision
The procedure centers on the use of an endoscope. This is a remarkably thin tube equipped with a lens and a powerful light source. It also contains a “working channel” through which specialized micro-instruments are passed. During the operation, high-definition monitors in the surgical suite provide the surgeon with a view that’s actually superior to the naked eye. These HD cameras offer incredible magnification and clarity. This allows for extreme precision when treating delicate neural structures. The use of these specialized tools ensures that every movement is targeted and controlled, minimizing the risk to nearby tissues.
Endoscopic vs. Microscopic Spine Surgery
Patients often ask how this differs from microscopic surgery. While microscopic techniques are certainly an improvement over open surgery, they still require a larger “corridor” to allow light to reach the surgical site. In contrast, endoscopic spine surgery places the camera directly at the point of the pathology. The use of angled lenses allows surgeons to see “around the corner,” reaching areas that would otherwise require significant bone removal or muscle retraction. By preserving more of the natural bone and ligament structures, we significantly lower the risk of post-operative instability. This precision is what makes a rapid return to normal activity a realistic expectation for our patients.
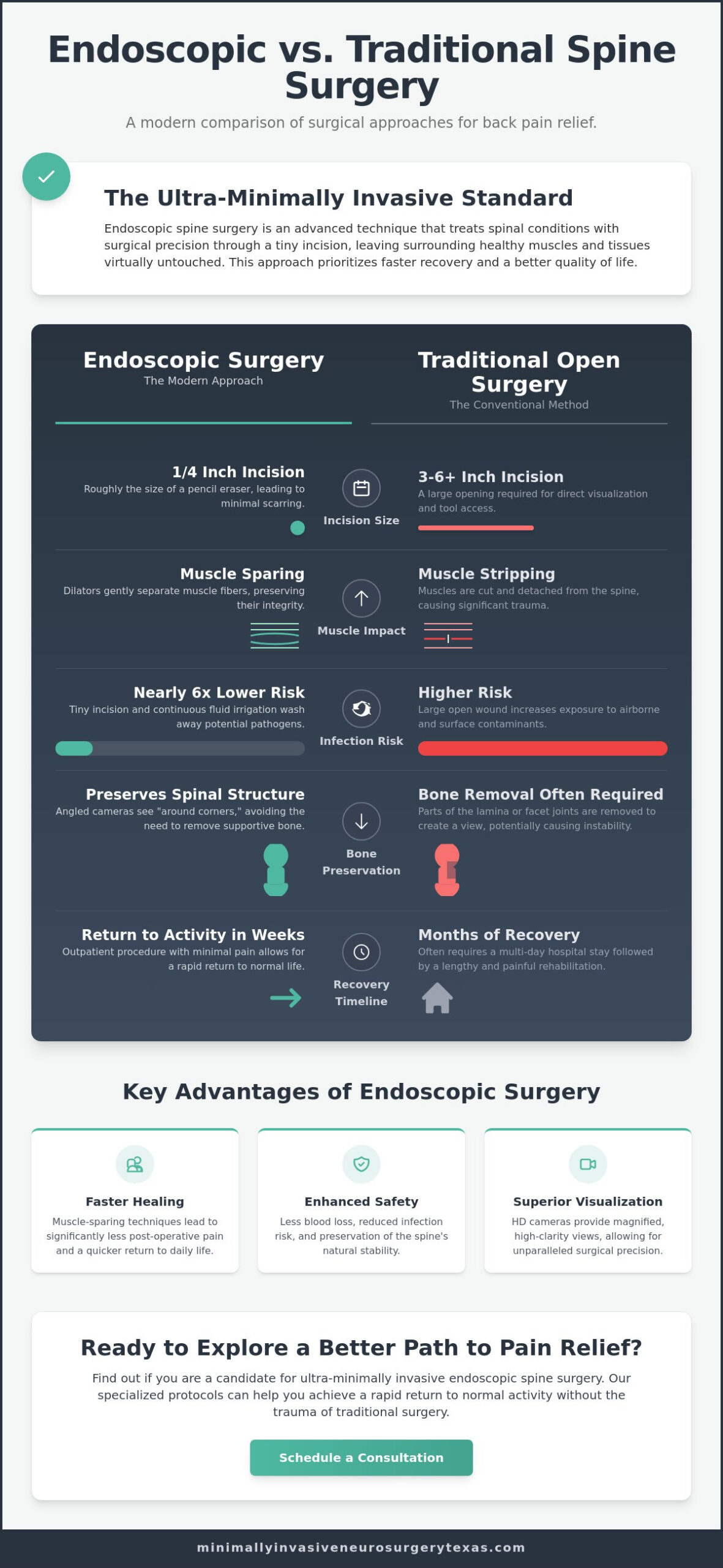
Endoscopic vs. Traditional Spine Surgery: A Comparison
Traditional spine surgery often requires a large incision and the detachment of significant muscle groups from the spine. This “muscle-stripping” approach is the primary cause of long-term post-operative pain and extended hospital stays. In contrast, endoscopic spine surgery represents the next evolution of Minimally Invasive Neurosurgery. Instead of cutting through tissue, the surgeon uses a series of dilators to gently push muscle fibers aside. This muscle-sparing technique preserves the natural anatomy and maintains the structural integrity of the back.
Patient safety is significantly enhanced through this precision. Because the incision is so small, blood loss is negligible. Additionally, the procedure utilizes continuous fluid irrigation. This constant flow of sterile saline keeps the surgical field clear and helps wash away potential pathogens during the operation. Research from a 2013 study indicates that these methods can reduce the risk of infection by nearly six times compared to traditional open surgery. This level of safety provides immense peace of mind for patients who are hesitant about the risks of major operations.
Structural Integrity and Bone Preservation
Maintaining the spine’s natural load-bearing capacity is a hallmark of the endoscopic approach. Traditional “open” procedures often require the removal of supportive bone, such as the lamina, just to gain a clear view of the affected nerves. This can compromise the stability of the spinal column over time. Endoscopy utilizes angled cameras to see around these structures. By preserving the facet joints and the lamina, we maintain the spine’s long-term health. This proactive approach often allows patients to avoid the need for a minimally invasive spinal fusion in the future. Protecting your original anatomy is our highest priority.
Anesthesia and Outpatient Benefits
The reduced physical trauma of endoscopic spine surgery changes the entire recovery narrative. Many of these procedures can be performed under conscious sedation rather than general anesthesia. This is a critical advantage for elderly patients or those with underlying health conditions that make general anesthesia risky. Without the “fog” of heavy sedation, patients recover more quickly and typically achieve a same-day discharge. Most individuals are back in the comfort of their own homes within hours of the procedure. This efficient, results-oriented flow is designed to help you achieve a rapid return to normal activity. If you are ready to explore these modern options, our team is here to guide you through the process of choosing the right surgical path.
Clinical Indications: Are You a Candidate for Endoscopic Surgery?
Determining if you are a candidate for endoscopic spine surgery begins with a shift in perspective. Many patients assume that a small incision is only suitable for minor back issues. This is a common misconception. Advanced visualization technology often allows us to treat complex pathologies that were previously unreachable without large, open incisions. However, it’s a specialized tool. It isn’t a “one-size-fits-all” remedy for every spinal condition. We rely on high-resolution MRI and CT imaging to act as a definitive roadmap. These scans reveal the exact location of nerve compression and the structural health of your vertebrae, allowing us to plan a targeted intervention.
Your diagnostic journey is the most critical phase of care. We look for a clear correlation between your physical symptoms and the findings on your imaging. If your pain is localized or radiating but stems from a specific, reachable area, endoscopy is often the superior choice. This precision ensures that we address the root cause of your suffering without disturbing the healthy segments of your spine. Our focus remains on providing a surgical solution that aligns with your specific lifestyle goals and physical needs.
Conditions Treated with Endoscopic Techniques
Endoscopic methods are exceptionally effective for treating herniated discs. We can specifically target foraminal protrusions, which are discs that bulge into the narrow exits where nerves leave the spinal canal. It is also a primary choice for treating spinal stenosis. By removing bone spurs or thickened ligaments through the endoscope’s working channel, we create necessary space for the nerves. This relieves the pressure causing chronic leg pain or sciatica. Because we can visualize the area in high definition, we can ensure the nerve is fully decompressed before the procedure concludes.
Candidacy Checklist for Plano Patients
Before considering surgery, we look for specific markers in your medical history. Most successful candidates share several characteristics:
- You’ve completed at least six weeks of conservative care, such as physical therapy or medication, without significant relief.
- Your pain radiates into your legs or arms, which typically suggests nerve root compression.
- Imaging confirms a structural issue, like a herniated disc or stenosis, that correlates with your symptoms.
- You’re seeking an alternative to traditional surgery to avoid the risks of extensive muscle damage.
Even if you’ve had a prior procedure and are suffering from “failed back surgery syndrome,” you may still be a candidate. Scar tissue from previous operations often makes traditional re-operation risky. The targeted nature of endoscopic spine surgery allows us to bypass old surgical sites and treat the problem directly. A consultation at our specialized center in Lewisville or Plano is the best way to confirm your eligibility. We’re here to help you move from a state of concern to a state of informed confidence as you pursue a return to normal activity.
The Patient Journey: Recovery and Outcomes at MINT
Your journey at MINT is designed to be as efficient and comfortable as possible. On the day of your endoscopic spine surgery, you’ll arrive at our specialized facility and typically return home within hours. The immediate post-operative period is characterized by rapid mobilization. Unlike traditional back surgery, which often leaves patients bedridden for days, we encourage you to walk shortly after the procedure. This early movement is vital. It prevents stiffness and promotes healthy circulation.
There is a profound psychological benefit to this approach. Seeing a single, small bandage instead of a large surgical wound significantly reduces patient anxiety. It reinforces the reality that your body has undergone a targeted intervention rather than a traumatic overhaul. This sense of optimism is a critical component of the healing process. Our boutique environment ensures you receive personalized attention during these crucial first 24 hours, moving you from a state of concern to a state of informed confidence.
Timeline for Returning to Daily Life
The recovery curve for endoscopic procedures is remarkably steep compared to traditional methods. During the first two weeks, you’ll focus on light activity. This includes walking and performing desk-based work. By weeks three through six, most patients experience a gradual increase in their physical capacity. This is when the milestone of a “return to normal activity” becomes a reality. Contrast this with the three to six month recovery window required for traditional fusion or open discectomy. Because we preserve the muscles and ligaments, your body doesn’t need to spend months repairing collateral damage.
Long-Term Success Rates
Clinical data supports the efficacy of these advanced techniques. Endoscopic discectomy typically sees success rates of approximately 90% for relieving radicular pain. Beyond the immediate results, the long-term benefits are equally significant. Because we preserve the natural bone structures, patients have a lower risk of “adjacent segment disease.” This is a common complication of traditional surgery where the levels above or below the surgical site wear out prematurely due to altered mechanics. To maintain these results, we provide specific post-operative ergonomic advice to help you protect your spine in the years to come.
If you’re ready to start your own journey toward relief, we invite you to schedule a consultation with our specialists to discuss your personalized path to recovery.
Choosing an Endoscopic Spine Specialist in Plano and Lewisville
Selecting the right surgeon is the most consequential decision you’ll make for your spinal health. While the technology behind endoscopic spine surgery is revolutionary, it remains a highly technique-dependent procedure. The precision required to operate through a 1/4-inch incision demands specialized training and significant experience. Dr. Scott Kutz has dedicated his career to mastering these advanced techniques, positioning MINT as a center of excellence for North Texas residents. By choosing a specialist who focuses exclusively on minimally invasive methods, you ensure that your care is managed by an expert who understands the nuances of tissue preservation.
Our boutique approach offers a distinct advantage over the bureaucracy of large hospital systems. In a specialized surgical center, every member of the clinical team is an expert in spine care. This creates a streamlined, patient-centered environment where your recovery is the primary focus. With convenient locations in both Plano and Lewisville, we provide high-tech surgical solutions right in your community. This accessibility reduces the stress of travel during your recovery, allowing you to focus entirely on your return to normal activity.
What to Ask Your Surgeon During a Consultation
Your consultation is an opportunity to verify that your surgeon operates at the forefront of modern medicine. We encourage patients to be proactive and ask direct questions about their care. Consider including these in your discussion:
- How many endoscopic procedures have you performed in the last year?
- What is your specific complication rate for this type of intervention?
- Do you utilize advanced robotic navigation systems like Globus Excelsius or Augmented Reality (AR) to enhance precision?
- Will my surgery be performed in a specialized outpatient spine center or a general hospital?
Confirming that your surgeon uses these proprietary technological systems signals that they are committed to the highest standards of safety and accuracy. These tools are hallmarks of a practice that operates at the absolute forefront of surgical innovation.
Why MINT is the Premier Choice for North Texas
At MINT, our focus is singular. We don’t divide our attention between cranial neurosurgery and spinal health. This specialization allows us to refine our protocols and achieve superior clinical outcomes for our back and neck patients. Our team combines clinical authority with a compassionate style, ensuring you feel supported from your initial diagnosis through your final follow-up. We’ve built our reputation on trust and the relief of suffering, acting as a source of optimism for those dealing with chronic pain. If you’re ready to move past failed conservative care, it’s time to explore your options with a leader in the field. Schedule your evaluation for endoscopic spine surgery in Plano today and take the first step toward reclaiming your quality of life.
Reclaiming Your Active Lifestyle with Precision Care
The evolution of spinal care has arrived in North Texas. You no longer have to choose between living with chronic pain and the trauma of traditional open surgery. By opting for endoscopic spine surgery, you’re choosing a path that preserves your natural anatomy and prioritizes a rapid return to normal activity. This ultra-minimally invasive standard offers a level of precision that was once unimaginable, allowing for targeted relief through an incision no larger than a pencil eraser.
At MINT, our focus is 100% on minimally invasive spinal care. Board-certified neurosurgeon Dr. Scott Kutz and his team utilize specialized outpatient surgery centers in Plano and Lewisville to ensure you receive high-tech care in a boutique, personalized setting. We’re dedicated to helping you move from a state of frustration to a state of informed confidence. Don’t let back pain dictate your future any longer. Request a Consultation with Dr. Scott Kutz at MINT today and discover how modern innovation can restore your quality of life. You deserve a recovery that’s as efficient as the surgery itself.
Common Questions About Endoscopic Spine Care
Is endoscopic spine surgery considered major surgery?
While any procedure involving the spinal column requires absolute precision, this approach is classified as an ultra-minimally invasive alternative to traditional major surgery. It avoids the extensive muscle trauma and large incisions that define open back operations. Because it’s typically performed in an outpatient setting with rapid discharge, it feels much less invasive to the patient than a multi-day hospital stay. You’ll experience the benefits of a targeted intervention without the systemic stress of a major inpatient reconstruction.
How long does the endoscopic spine procedure take?
Most endoscopic procedures are completed within 60 to 90 minutes. The exact duration depends on the complexity of your specific condition and the number of levels being treated. Because the surgeon uses high-definition visualization to navigate directly to the problem area, the time spent in the operating suite is significantly reduced compared to complex open surgeries. This efficiency is a hallmark of our results-oriented approach to spinal health.
Will I have a scar after endoscopic surgery?
Scars are typically minimal and often fade significantly over time. The incision required for endoscopic spine surgery is only about 1/4 inch wide, which is roughly the size of a pencil eraser. Most patients find that the site is easily covered by a standard adhesive bandage. This small entry point is a primary reason why post-operative scarring is negligible compared to the large, visible scars left by traditional methods.
What is the success rate of endoscopic spine surgery compared to traditional methods?
Clinical outcomes are excellent, with success rates for endoscopic discectomy reaching approximately 90% for relieving nerve-related pain. This matches or exceeds the results of traditional open surgery while offering the added benefits of a faster recovery. Additionally, research indicates these methods can reduce the risk of infection by nearly six times compared to traditional open surgery. By preserving the natural bone and muscle structures, we also improve the long-term stability of your spine.
Can endoscopic surgery fix a herniated disc permanently?
This procedure is designed to provide a permanent solution by removing the specific portion of the disc that’s compressing your nerves. While we can’t stop the natural aging process of the rest of the spine, the targeted decompression effectively resolves the immediate structural cause of your pain. Following our post-operative ergonomic advice is essential for maintaining the long-term health of your spinal discs and preventing future issues.
How soon can I drive after having endoscopic back surgery?
Most patients can resume driving within one week of the procedure. You must be completely finished with any narcotic pain medications and feel physically capable of making sudden movements or braking safely. We provide specific clearance during your first follow-up appointment to ensure you’re ready for a safe return to normal activity behind the wheel. Your safety and the safety of others remain our top priority during this transition.
Does insurance typically cover endoscopic spine procedures in Texas?
Most major insurance plans in Texas, including Medicare, cover these procedures when they’re deemed medically necessary. Coverage details vary between providers like Blue Cross Blue Shield, Aetna, Cigna, and United Healthcare. It’s important to verify your specific benefits, including deductibles and co-pays, with your insurance carrier. Our team can assist in checking your coverage for endoscopic spine surgery during your initial consultation to ensure you have informed confidence in your care plan.
Is endoscopic spine surgery painful during recovery?
Patients generally report significantly less pain during recovery compared to traditional open surgery. Because we don’t cut or strip the back muscles, the primary source of post-operative suffering is eliminated. Most individuals manage any minor discomfort at the incision site with over-the-counter medications or a short course of mild prescriptions. This reduced physical impact is what allows for such a rapid healing process and a faster return to your daily routine.