Approximately 25% of the general adult population currently lives with an intervertebral disc protrusion, yet most only realize there is a problem when chronic radiating pain or sciatica begins to limit their mobility. If you are staring at an MRI report filled with technical jargon, it’s easy to fear that a bulging disc means a permanent disability or a lifetime of restricted activity. You aren’t alone in feeling overwhelmed by terms like “annular tears” or “nerve impingement,” especially when your primary goal is simply to wake up without discomfort and enjoy your day.
This guide clarifies the critical differences between bulging and herniated discs, helping you decode your diagnosis with clinical confidence. We’ll explore the transition from conservative care to modern, ultra-minimally invasive techniques, including advancements like the Arthrex technology released in late 2025 that allows for surgical incisions smaller than one centimeter. By understanding the full spectrum of 2026 treatment options, from regenerative therapies to precision-guided MISS, you can move past the confusion and find the right path to get back to life.
Key Takeaways
- Understand why a bulging disc is considered a contained structural shift and how the “jelly donut” analogy helps distinguish it from a true herniation.
- Identify the specific symptoms of radiculopathy to understand why a spinal condition often causes radiating pain, numbness, or tingling in your legs.
- Recognize the lifestyle factors and repetitive stresses, such as “tech neck,” that accelerate disc dehydration and lead to premature spinal wear.
- Discover how advanced robotic platforms like Globus Excelsius provide the sub-millimeter precision necessary for successful minimally invasive outcomes.
- Learn the criteria for moving from conservative management to specialized surgical interventions designed to help you get back to life quickly.
What Is a Bulging Disc? Understanding Spinal Anatomy
A bulging disc occurs when the tough outer wall of a spinal disc weakens, causing the disc to extend beyond its normal boundary into the spinal canal. Think of your spinal discs as the high-performance shock absorbers of your body. They sit between your vertebrae, providing the necessary cushion to handle the daily stresses of walking, lifting, and gravity. Without these discs, your vertebrae would grate against each other, causing immediate and severe damage to the skeletal structure.
Findings on an MRI can be intimidating, but these structural shifts are common. Data published on January 30, 2026, shows that intervertebral disc protrusion affects about 25% of the general adult population. Many people live with these results without experiencing any pain. Discomfort only begins when the bulge creates mechanical pressure on the spinal cord or the sensitive exiting nerve roots. This pressure often manifests as:
- Persistent, localized aching in the neck or lower back
- Radiating numbness or tingling that travels into the extremities
- Muscle weakness that affects your grip or your ability to walk
The Role of Spinal Discs as Shock Absorbers
The internal mechanics of a disc depend on the nucleus pulposus, which is a gel-like inner core that provides hydraulic resistance to vertical pressure. This core allows the cervical and lumbar spine to remain flexible while distributing weight evenly across the vertebral column. The annulus fibrosus is the protective circular exterior of the intervertebral disc. When this exterior loses its shape, the resulting protrusion narrows the space available for nerves, often leading to the radiating discomfort that keeps you from your favorite activities.
Bulging vs. Herniated Disc: The Key Distinctions
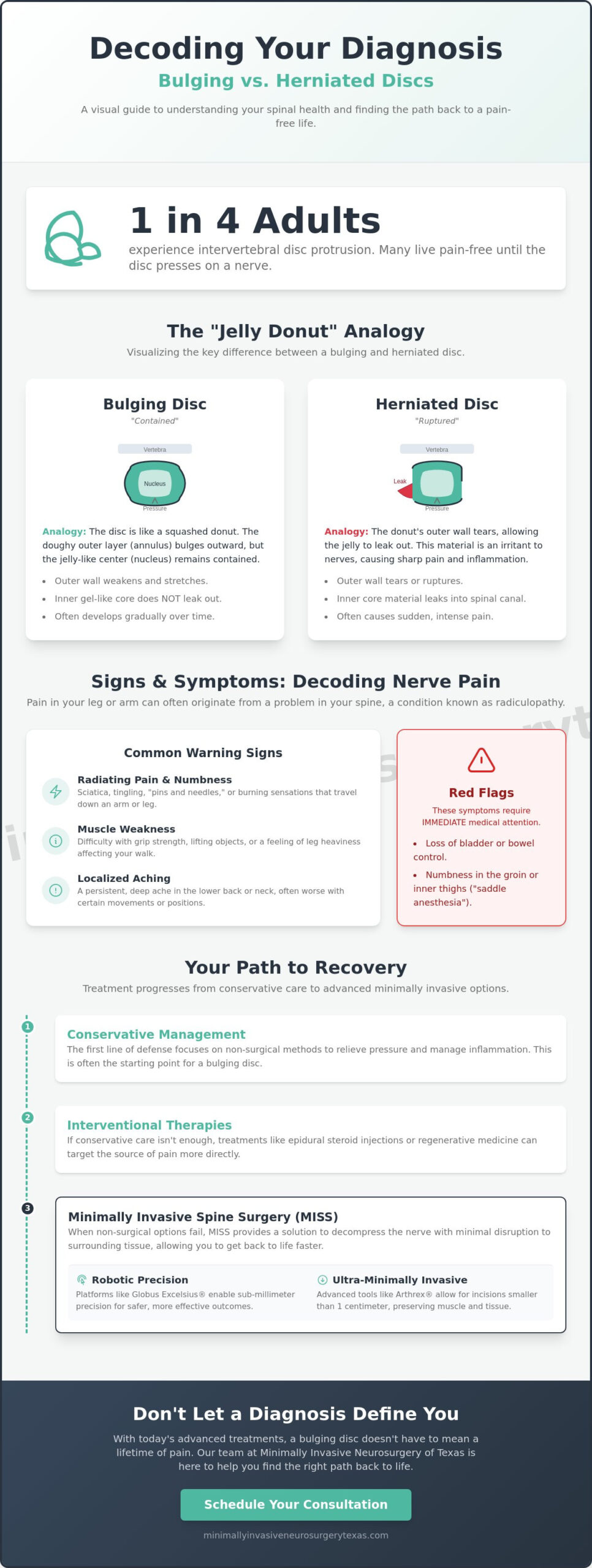
We often use the “jelly donut” analogy to help patients visualize the difference between these two conditions. A bulging disc is like a donut that has been slightly compressed; the dough pushes outward, but the jelly stays contained inside. In contrast, a Spinal disc herniation happens when the outer layer actually ruptures, allowing the internal “jelly” to leak out. This distinction is vital because it dictates your clinical path and the urgency of the intervention.
Herniations usually cause sudden, sharp pain because the leaked material triggers an intense inflammatory response against the nerves. Bulges tend to be more gradual, often resulting from years of natural wear or repetitive stress. Because the bulge is contained, we often start with conservative management to see if the body can adapt. If those methods fail to provide relief, we utilize MISS (Minimally Invasive Spine Surgery) to decompress the nerve with sub-millimeter precision. Don’t let a diagnosis of a bulging disc stop you; our advanced techniques are designed to help you get back to life quickly and safely.
Identifying Bulging Disc Symptoms and Warning Signs
Many patients are surprised to learn that the source of their leg or arm pain is actually located in their spine. This phenomenon, known as radiculopathy, occurs when a bulging disc compresses a nerve root at its origin. While localized back pain is common, the most debilitating symptoms are often distal, meaning they occur far from the actual site of the protrusion. Understanding how these signals travel is the first step in regaining control of your health.
Sensory changes are frequently the first warning signs. You might feel “pins and needles,” a persistent tingling, or even phantom sensations of intense heat or cold in your extremities. These neurological signals indicate that the nerve is under mechanical stress. If left unaddressed, these sensations can progress into significant muscle weakness or a loss of coordination. Because every patient’s anatomy is unique, a local specialist can help correlate your specific symptoms with your imaging results.
Certain red flags require immediate medical intervention. If you experience “saddle anesthesia,” which is numbness in the groin and inner thighs, or a sudden loss of bladder or bowel control, you must seek emergency care. These symptoms can indicate cauda equina syndrome, a rare but serious condition where the nerve roots at the base of the spinal cord are severely compressed.
Lumbar Bulging Disc Symptoms (Lower Back)
The lumbar region is the most frequent site for disc issues because it bears the majority of your body weight. Sciatica is the hallmark symptom here. It’s often described as a searing or electric shock-like pain that travels from the buttock down the back of the leg. Approximately 450,000 to 500,000 discectomies are performed in the United States each year, largely to address these types of lumbar issues. You might also notice muscle weakness in the feet or knees, sometimes leading to “foot drop,” where you struggle to lift the front of your foot while walking. This pain typically worsens during activities that increase spinal pressure, such as sitting for extended periods, coughing, or sneezing.
Cervical Bulging Disc Symptoms (Neck)
When a bulging disc in the neck protrudes, the pain radiates into the shoulders, arms, and fingertips. You might notice a subtle loss of fine motor skills; tasks like buttoning a shirt or typing become noticeably difficult. Chronic headaches originating from the base of the skull are another frequent indicator of cervical nerve compression. Reviewing Herniated Disk Symptoms & Treatment guidelines can provide additional context on how these symptoms differ from localized muscle strain. Identifying these patterns early is essential to implementing a plan that helps you get back to life.
Common Causes and Risk Factors for Disc Protrusion
A bulging disc is rarely the result of a single, isolated incident. Instead, it’s often the culmination of gradual structural changes that occur over several years. While aging is the primary driver, lifestyle choices and environmental stressors in the North Texas area play significant roles in how quickly these changes progress. Understanding these factors is essential for both prevention and choosing the right path for treatment.
Age-related degeneration is the most common cause. Your spinal discs are composed of approximately 80% water at birth, but they naturally dehydrate over time. This loss of fluid makes the discs less pliable and more prone to shifting under the weight of the body. Data published on January 30, 2026, indicates that low back pain affects up to 80% of individuals at least once in their lifetime, with disc pathology accounting for a significant portion of these cases. Genetic predisposition also plays a role; if your parents suffered from degenerative disc disease, you may be more susceptible to similar issues.
Repetitive stress and acute injuries are also major contributors. In Plano’s professional environment, “tech neck” has become a pervasive issue. Maintaining a forward-leaning posture while using mobile devices or computers increases the mechanical load on the cervical spine, accelerating wear. High-impact events, such as sports injuries or vehicular accidents on the DFW North Tollway, can also cause a sudden protrusion of disc material.
Lifestyle Factors and Prevention
Your daily habits significantly impact spinal health. Obesity increases the constant axial load on the lumbar spine, forcing the discs to work harder to maintain stability. Smoking is another critical risk factor. It constricts the small blood vessels that supply essential nutrients to the spinal discs, which impairs the body’s natural ability to heal small tears in the annulus fibrosus. For office workers in Plano and Lewisville, implementing ergonomic best practices, such as using standing desks and maintaining a neutral spine position, can mitigate these risks and help you avoid chronic pain.
The Diagnostic Journey: From MRI to Specialist
Getting an accurate diagnosis is the first step toward recovery. While an X-ray can rule out bone fractures, it’s unable to show the soft tissue of the disc itself. An MRI is the gold standard for identifying a bulging disc. When you review your report, you might see terms like “effacement,” which means the disc is pressing against the protective sac around the nerves, or “foraminal stenosis,” which refers to the narrowing of the holes where nerves exit the spine. We prioritize a clinical correlation, which means we match your imaging results with your actual physical symptoms. We treat the patient, not just the picture, to ensure you receive the precise care needed to get back to life.
Treatment Roundup: From Conservative Care to MISS
Most patients diagnosed with a bulging disc find relief through a structured protocol of conservative care. This first-line defense typically includes targeted physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs), and activity modification. Clinical guidelines in 2026 suggest a 6 to 12-week window for these methods to work before considering more advanced interventions. During this period, the goal is to manage inflammation and strengthen the supporting musculature of the spine to reduce the mechanical load on the affected disc.
Epidural Steroid Injections (ESIs) often bridge the gap between medication and surgery. By delivering powerful anti-inflammatory agents directly to the site of nerve compression, ESIs reduce swelling and buy time for the body’s natural healing processes to take effect. While injections don’t physically “fix” the bulge, they provide the necessary pain relief for patients to participate more effectively in physical therapy, which is essential for long-term stability.
When conservative paths fail to provide relief, the conversation shifts to surgical intervention. It’s vital to understand that there’s a profound difference between traditional open back surgery and MISS (Minimally Invasive Spine Surgery). Traditional methods often require incisions of three to five inches and the detachment of significant muscle tissue. In contrast, our approach utilizes specialized dilators and robotic guidance to access the spine without unnecessary trauma. This precision is why the success rate for procedures like microdiscectomy remains high, ranging between 75% and 95% as of July 2025. A bulging disc doesn’t have to mean a long, painful recovery if you choose the right surgical path.
Minimally Invasive Surgical Options
A microdiscectomy remains the gold standard for relieving nerve pressure through a tiny incision. For even more precise needs, endoscopic spine surgery offers “keyhole” access that preserves nearly all surrounding tissue. We also specialize in artificial disc replacement, a field that has seen massive growth, with the market for these devices expected to reach $1.47 billion in 2026. This procedure allows for continued spinal mobility, avoiding the rigidity often associated with traditional spinal fusion. New technology from Arthrex, available since late 2025, even allows for ultra-minimally invasive discectomies through incisions smaller than one centimeter.
Recovery Expectations in 2026
Modern neurosurgery has transformed the patient experience. Most MISS procedures are now performed on an outpatient basis, meaning you can typically go home the same day. Patients experience significantly less post-operative pain and minimal blood loss compared to traditional techniques. For insured patients, out-of-pocket costs for these life-changing procedures typically range from $1,500 to $6,000. You can learn more about what to expect following your procedure by reviewing our guide on Recovery Times for Minimally Invasive Spine Surgery. If you are ready to stop managing pain and start living again, schedule a consultation with our specialized team today.
Why Choose MINT for Bulging Disc Treatment in North Texas
Choosing the right specialist for a bulging disc is a decision that directly impacts your long-term mobility and quality of life. At Minimally Invasive Neurosurgery of Texas (MINT), we combine the clinical authority of board-certified expertise with a compassionate, patient-centered approach. Dr. Scott Kutz has dedicated his career to the specialized field of minimally invasive neurosurgery, ensuring that patients in the DFW metroplex have access to world-class care. Our practice is built on the belief that surgical precision leads to superior outcomes, and we prove this daily at our clinics in Plano and Lewisville.
We believe that healthcare should be accessible and community-focused. By maintaining a boutique surgical center environment, we avoid the coldness of large hospital systems. This allows our team to provide personalized attention and a clear, results-oriented path for every individual we treat. From the moment you enter our facility, your health is our top priority, and our goal is to move you from a state of concern to a state of informed confidence.
The MINT Difference: Robotic and AR Precision
Robotic navigation platforms like the Globus Excelsius represent the absolute forefront of modern spinal care. This technology allows for sub-millimeter precision during complex reconstructions, significantly increasing safety by providing real-time, 3D feedback to the surgical team. We also utilize Augmedics AR, which functions as a high-tech “GPS for the spine” by overlaying a patient’s diagnostic imaging directly onto their anatomy through specialized headsets during the procedure. Robotic-assisted surgery at MINT reduces tissue disruption for faster patient recovery. By minimizing the impact on surrounding muscles and ligaments, we help you transition from the operating room to your recovery at home with greater speed and less post-operative discomfort.
Getting Back to Life in Plano and Lewisville
We understand that a diagnosis of a bulging disc often comes with a fear of permanent nerve damage and a loss of hope. Our mission is to reverse that narrative by guiding you through a successful recovery arc. We’re committed to helping our patients enjoy every single day of their lives by utilizing the most innovative MISS techniques available in 2026. Whether you are struggling with chronic sciatica or cervical nerve compression, our specialized team provides the beacon of hope you need to overcome suffering. If you are ready to reclaim your mobility and leave chronic pain behind, Schedule a consultation with Dr. Scott Kutz today and discover the MINT difference.
Take the Next Step Toward Lasting Relief
Living with a bulging disc doesn’t have to mean accepting a future of limited mobility or chronic pain. As we’ve explored, the transition from conservative management to modern surgical precision is now safer and more efficient than ever. With success rates for microdiscectomy reaching up to 95% as of July 2025, the medical landscape in 2026 offers clear, proven paths to recovery. By combining clinical authority with the latest innovations, you can move from a state of concern to a state of informed confidence.
Board-certified neurosurgeon Dr. Scott Kutz and the specialized team at MINT utilize the Globus Excelsius robotic navigation system to ensure sub-millimeter accuracy during every procedure. Our boutique surgical centers in Plano and Lewisville prioritize your personal attention and recovery journey over the coldness of large hospital systems. It’s time to stop letting spinal discomfort dictate your schedule and start enjoying every single day of your life again.
Get Back to Life-Schedule Your Consultation at MINT today. Your path to a pain-free future is just a specialized diagnosis away.
Frequently Asked Questions
Can a bulging disc heal on its own without surgery?
Most patients experience significant improvement through conservative care within six weeks of their initial diagnosis. Approximately 90% of individuals find that their symptoms resolve as the body adapts to the structural shift or the inflammation around the nerve root subsides. If your pain persists beyond the 12-week mark, a specialist evaluation is necessary to prevent chronic nerve irritation and determine if a more advanced intervention is required.
How do I know if my back pain is a bulging disc or just a muscle strain?
Muscle strains typically cause localized discomfort that resolves with rest, whereas a bulging disc often triggers radiating symptoms like sciatica. If your pain travels into your glutes or legs, or if you experience persistent numbness and tingling, it’s likely a neurological issue rather than a soft tissue strain. Diagnostic imaging remains the only definitive way to confirm the source of your discomfort and rule out permanent nerve impingement.
What is the most successful treatment for a bulging disc in the lower back?
Microdiscectomy is the gold standard for patients who fail to find relief through conservative management. Data from July 2025 indicates this procedure has a success rate between 75% and 95% for appropriately selected candidates. At MINT, we utilize robotic navigation and MISS techniques to ensure sub-millimeter precision, which allows patients to get back to life with minimal downtime and a significantly reduced risk of recurrence compared to traditional open surgery.
Is walking good for a bulging disc, or should I rest?
Walking is generally beneficial because it promotes essential blood flow and maintains spinal flexibility. Prolonged bed rest can actually stiffen the spine and weaken the supporting musculature, which often worsens the underlying condition. We recommend short, frequent walks on flat surfaces while avoiding high-impact activities. This gentle movement helps maintain the hydraulic function of the discs without adding excessive axial load to the vertebrae.
What happens if a bulging disc is left untreated for too long?
Untreated nerve compression can lead to permanent neurological damage, muscle atrophy, or chronic pain syndromes. Over time, the constant pressure on a nerve root can cause a loss of sensation or motor function in your extremities. In severe cases, a neglected protrusion can progress into cauda equina syndrome. This is a medical emergency that requires immediate surgical intervention to prevent permanent paralysis or loss of bladder control.
How long does it take to recover from minimally invasive surgery for a bulging disc?
Most patients return to light daily activity within one to two weeks following a MISS procedure. Because our techniques involve incisions smaller than one centimeter, the disruption to surrounding tissue is minimal. While every recovery is unique, many DFW professionals return to office work in approximately 10 days. We provide a structured recovery plan to ensure you regain your strength safely and quickly.
Are there specific exercises I should avoid with a bulging disc?
You should avoid heavy lifting, toe touches, and high-impact sports that involve jumping or running. These movements increase the pressure on the annulus fibrosus and can exacerbate the bulging disc. Exercises that require heavy spinal rotation or twisting should also be avoided until a specialist clears you for such activity. Focus instead on low-impact movements that stabilize your core and protect the integrity of your spinal column.
Can a bulging disc cause pain in other parts of the body like the hips or legs?
Referred pain in the hips, glutes, and legs is one of the most common indicators of a lumbar disc issue. This occurs because the protruding disc material presses on the sciatic nerve, which is the largest nerve in the human body. While you may feel the most intense pain in your leg, the mechanical problem is located in your spine. Correcting the spinal compression is the only way to resolve these radiating symptoms permanently.



